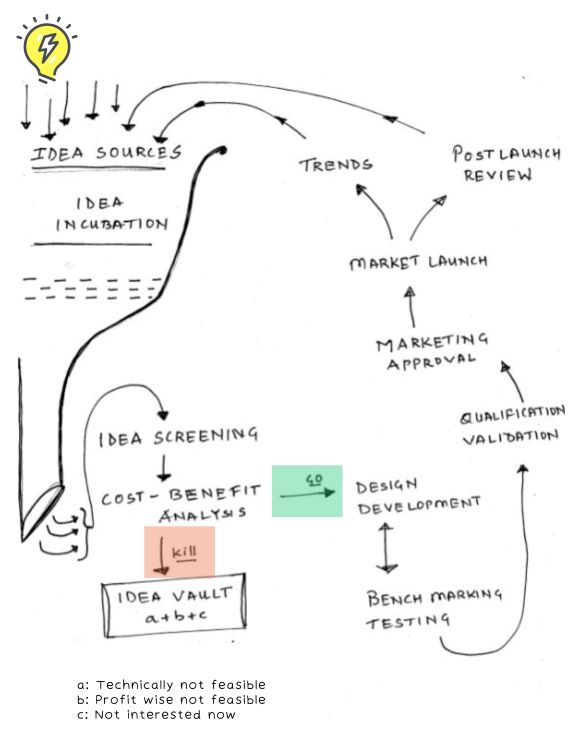
There are several types of machine learning, but broadly there are two types of machine learning: Supervised ML and Unsupervised ML.
Unsupervised machine learning aims to find patterns in unlabeled data, while supervised machine learning looks for trends in labels. In this post, I shall touch upon what is machine learning, where is machine learning used, benefits & challenges of machine learning and few examples of its industry applications. So, let’s get started…
Industrial uses of machine learning:
Machine learning is an innovation and is used in Industry 4.0 or smart factories.
Machine learning is a vey powerful tool for business. It helps business leaders to predict customer demands, price products and segment customers. It also helps to forecast inventory levels and detect fraudulent activities. Machine learning’s capabilities range from image recognition to natural language processing. Businesses that rely on these technologies can provide better customer service, improve security, and even allow consumers to complete transactions without a human being. These innovations are changing the way we buy and sell goods.
Machine learning can be used to predict which products and services are best for a customer. Streaming service companies and social media apps use recommendation engines that analyze data to make recommendations based on personal preferences. Enterprises also use AI to predict customer churn. This allows them to better serve their customers and maximize profits.
Application of machine learning concept to technical and business processes improves operational excellence and in turn, increases profitability.
Which industries will benefit most from machine learning?
Transportation industry for now. The transportation & logistics industry perhaps uses machine learning the most. Reinforcement machine learning trains models through trial and error and is often used to teach autonomous vehicles how to drive. It rewards the machine when it makes the right decisions.
Advantages and disadvantages of machine learning:
Some of the advantages of machine learning include the ability to customize education, which allows students to work on materials that are most suitable for their learning style. This can save teachers time because they do not have to plan a lesson for every student. Another benefit is an automatic grading system, which saves teachers time and gives a realistic assessment of student performance.
However, this technique requires a large amount of data to function properly. This is not only a time-consuming task, but it also requires resources such as CPU and GPU power. Furthermore, it may use more storage space than expected. In addition, machine learning algorithms can only be used as much as they have historical data to work with.
Another advantage of machine learning is that it allows for fast and automatic adaptation, which eliminates the need for human intervention. This feature is also used in anti-virus software and security software, which can automatically adapt to any situation without human intervention. The downside of machine learning is that it can sometimes make mistakes, causing inaccurate predictions or inaccurate advertising.
Challenges of machine learning:
Machine learning has a wide range of implications. Its use in making decisions can have a huge impact on the economy and our everyday lives. Research in this field is aimed at understanding the impacts and potential harms of machine-learning-based systems and developing tools and policies to avoid them. It also examines the optimal use of machine-learning systems to maximize aggregate social welfare.
Machine-learning specialists face many challenges in the deployment of their projects. Sometimes the algorithms they use are not accurate enough to solve a business problem. In this case, the project may fail. To avoid such scenarios, it is vital to have a team of experts with business qualifications working on the project. This will enable organizations to make the best use of this new technology and get faster ROL
In addition, organizations are under pressure to only develop machine-learning models that produce a positive ROI. The ROI of a model can depend on how users react, as well as how well it predicts the future. Moreover, it can be impacted by competition, public opinion, brand image, and algorithmic fairness.
Examples of machine learning in action:
Predictive analytics is one of the most exciting examples of machine learning in action. It can be used to make predictions about a wide variety of things, from real estate prices to product development. Machine learning algorithms use big data to make these predictions. They do this by analyzing billions of data samples and automating the process of annotating them.
Another great example of machine learning in action is the social media news feed. The recommendation engine in the news feed uses machine learning to recommend articles based on the user's past browsing behavior. This kind of learning is possible because the algorithms are able to improve their accuracy over time as they are used more.
Machine learning has found wide-spread applications in drug discovery & biomedical research, and improving operational excellence in financial institutions, healthcare, IT, transportation & logistics, retail & e-commerce, agriculture, aviation and education industry verticals. I shall be covering these in-depth in my upcoming book on Machine Learning. The book will highlight how Machine Learning can be used to improve operational excellence in manufacturing and service industries. It will feature on Amazon, so do plan to check it out.
Related Reading:
- Continuous improvement tools
- How to cut costs strategically using Kaizen
- Streamline processes and workflows with Gemba Walk.
- Top Ten Strategic Decision-Making Tools for Operational Excellence
Follow Shruti on Twitter, YouTube, LinkedIn
Categories: Innovation | Operational Excellence | Machine Learning
Keywords and Tags:
#operationalexcellence #AI #ML #artificalintelligence #innovation #machinelearning #whatismachinelearning #machinelearningintrasportationindustry #profitability